Vital
The Government Health Plan “Vital” is responsible for providing physical and mental health services to 1.3 million Puerto Ricans. Services are offered by provider networks (primary doctors, specialists, hospitals, laboratories, etc.) throughout the island.
Important phone numbers:

Beneficiary Services
1-866-600-4753 (Toll-free)
1-844-726-3345 (TTY (hearing impaired)
TeleCuidado Menonita (Medical Advice Line)
1-844-736-3345 (Toll free)
1-844-716-3345 TTY (hearing impaired)
www.MenonitaVital.com

Medicaid Program Call Center
787-641-4224

ASSMCA (Linea PAS)
Mental Health Service Line
1-800-981-0023

Patient Advocate Office
Toll-free 1-800-981-0031
TTY 787-710-7057

Puerto Rico Health Insurance Administration (ASES)
VITAL
Toll-free 1-800-981-2737
TTY 787-474-3389

Do you want to change insurance?
VITAL
1-866-280-2053
1-888-984-0128 (TTY)
1-833-253-7721 (Spanish)
www.PlanVitalPR.com
For information about Vital: www.asespr.gov
For information about Medicaid programs: www.medicaid.pr.gov
For more information on patient protections: www2.pr.gov/Directorios
Who can apply to Vital?
Everyone can apply voluntarily.
NOTE: Foreigners with permanent residence permits in the United States have a waiting period to apply for benefits if the permit was granted after August 22, 1996.
Where to apply?
To apply:
- Call the Medicaid Call Center at (787) 641-4224 / (787) 625-6955 TTY (hearing impaired). Monday through Friday from 8:00 am to 6:00 pm to request an evaluation appointment
- Also, visit the Medicaid webpage: www.medicaid.pr.gov
Documents you must provide when you go to your appointment in the Medicaid Program
- Photo Identification Card (eg driver’s license, voting card)
- Original and copy of the Social Security Card (of all the members of the family unit)
- If you receive income from Social Security
- If you receive pension income (retirement, veterans, military or disability)
- Copy of Marriage Certificate (if applicable)
- Evidence of studies of children living in the home
- Water, Light or Telephone billing statements
- If you are pregnant, copy the pregnancy test
- If divorced or separated, bring evidence
- If you are a foreigner
Obtain the necessary documents to complete your application and present it to our offices. Complete them, print them and visit Medicaid office in your Municipality.
Information you must provide when you go to Medicaid
- If you receive income through:
- Work
- Social Security
- Pension
- Other
- If you have drug expenses
- If you are pregnant
NOTE: Additional information and/or documentation to those mentioned here may be requested according to your situation.
Determination of eligibility
In order to review your benefits application and be evaluated in accordance with current rules and procedures:
- Go to your appointment on the corresponding day and time.
- Arrive at your appointment 15 minutes in advance.
- Be sure to bring all the documents requested to you.
What if you have a newborn?
If you have a newborn, visit your Medicaid Office and give them a copy of the newborn’s birth certificate to enroll the newborn in Vital. If you do not do this, the newborn cannot get services under Vital. Furthermore, when you have a newborn, you also might be able to get other benefits, so it is important to visit the Medicaid Office, so they can check.
How to keep Vital benefits?
To keep your Vital benefits, you have to go to all your Medicaid appointments. Plan de Salud Menonita will send you a letter 90 days, 60 days and 30 days before the day when your Vital benefits stop. These letters will remind you that you have to go to your local Medicaid Office to maintain your eligibility in Vital.
If you miss your appointment, call the Medicaid Program Call Center at 787-641-4224 or visit your local Medicaid Office to ask for a new appointment.
This is your ID Card with Plan de Salud Menonita


Each insured person in your family will have his/her own ID card, even if he/she is a newborn. Your ID card has important information like:
- Your ID number (MPI)
- How to access emergency services
- Any money you will pay for health services
- The phone number for the free MI Salud (ASES) Service Line
- PMS Beneficiary Services line
- and the free 24/7 PSM Medical Advice Line: TeleCuidado Menonita
If you need to use your health benefits before you get your ID card, use your MA-10 form given to you by your Medicaid Office.
Remember to:
- Always carry your ID card with you
- Keep your card in a safe place so you don’t lose it
- Take your ID card when you go to the doctor or to the emergency room
- Be sure they give you your ID card back
Important to remember: first, your ID card is only for you. Second, don’t let anyone else use your card. Third, if your card is lost or stolen, you can ask your Insurer for a new card.
You can visit any of the PSM Service Centers or call the PMS Beneficiary Service line at 1-866-600-4753 (free of charge)/ 1-844-726-3345 TTY (hearing impaired).
How to choose an insurer?
Once you sign up for Vital, you can choose your Insurer. Your Insurer will work with you and your doctors to keep you healthy.
There is an enrollment counselor available in Medicaid offices and on the phone, who can help you choose an Insurer. The enrollment counselor does not work for any Insurer or any providers. They are neutral. They can give you information about Vital and your benefits. They can tell you about the choices available to you and help answer your questions. They can’t choose for you. They can help you:
- Choose a new Insurer or change Insurers;
- If you change your Insurer, they can also help you change your Primary Care Physician (PCP) or Primary Medical Group (see more information in Part 2 of the Beneficiary Manual).
You can contact the Enrollment Counselor for support:
- By phone at 787-641-4224, Monday through Friday, 8 am to 6 pm
- In the Medicaid offices
There are Enrollment Counselor staff in each of the Medicaid Offices. The offices are open Monday through Friday from 7:30am to 4:00pm. Your Insurer can tell you the Medicaid Office that is closest to you.
If you do not choose an Insurer, one will be chosen for you.
Can you change the insurer?
Yes, you can ask to change your Insurer. Once you have chosen an Insurer or one has been chosen for you, you have 90 days to change Insurers. You can also change your Insurer once a year during the “open enrollment period”, which is from November 1 to January 31.
If you want to change your Insurer, call the Enrollment counselor at 787-641-4224 or visit your local Medicaid Office.
You can also ask to change your Insurer at any time if you have certain reasons, like:
- You are not able to access services or providers
- You cannot get all related services you need at one time from the doctors, healthcare professionals and service facilities that work with your Insurer.
- You get poor-quality care
- You ask for a service that your Insurer does not cover because of moral or religious reasons.
- Your Insurer does not have doctors that are experienced in dealing with your health care needs
If you want to change your insurer for one of these reasons, you can ask for this change from the Insurer, the enrollment counselor or ASES. ASES will decide if you can change or if you have to wait until Open Enrollment. If you do not like the decision ASES makes, you can ask them to reconsider. If the decision is still not to your liking, you can ask for a hearing.
Can the membership with your insurer stop?
Yes, your membership with your Insurer will stop if you:
- Lose eligibility for Vital
- Move outside of Puerto Rico
- Go to prison
- Give your ID card to someone else to use
- Move to a long-term care nursing facility or intermediate care facility for the developmentally disabled
You will not lose your membership with your Insurer if:
- You have changes in your health
- You are using more health care services
You also might want to stop your membership with your Insurer if you no longer need your Vital benefits. If this happens, let your Medicaid Office and your Insurer know.
How to report changes?
Vital and your Insurer are committed to helping you. To support your needs, we need your help.
Please remember to let your Medicaid Office and Insurer know of any changes that may affect your membership or benefits. Some examples include:
- You are pregnant.
- You have a newborn
- You have changes in your family group (for example, you get married, someone in your family dies, and someone in your family reaches age 21)
- You move or your phone number changes
- You or one of your children has other health insurance
- You have a special medical condition.
- You move outside of Puerto Rico
- Your income changes (for example, you lose your job or get a new job)
To report a change, call the Medicaid Program call center at 787-641-4224 or visit your local Medicaid Office.
It is important to make sure your contact information is up to date with your local Medicaid Office. This is important because Medicaid and your Insurer send you important information about your Vital coverage and benefits in the mail. Most importantly, if they don’t have your current address, you could lose your Vital benefits. To report a change, call your Insurer or visit your local Medicaid Office.
Sometimes you will have to pay to get health care services. Preventive Care is care that helps you stay well, like checkups, shots, pregnancy care, and childbirth. This kind of care is always free. You don’t have copays for preventive care.
For other care like hospital stays or sick child visits, you may have to pay part of the cost. Copays are what you pay for each health care service you get.
Not everyone in Vital has copays. Your ID card will tell you if you have copays and what they are. Copays depend on the type of Vital you have. Your ID card says what type of Vital you have.
None of your doctors or providers can refuse to give you medically necessary services because you don’t pay your copays. But, your Insurer and your providers can take steps to collect any copays you owe.
You should only have to pay your copay for the services received. You should not be billed for the rest of the cost of your care. If you are billed for the rest of the cost, you can appeal. Click here for information on how to make an appeal.
Copayment Charts
Do you have to pay copays for a PCP, Specialist, ER visit, hospital stay, or other type of service? Not sure?
Check the chart below, look at your ID card or call the PSM Beneficiary Service line at 1-866-600-4753 (free of charge)/ 1-844-726-3345 TTY (hearing impaired) for information.
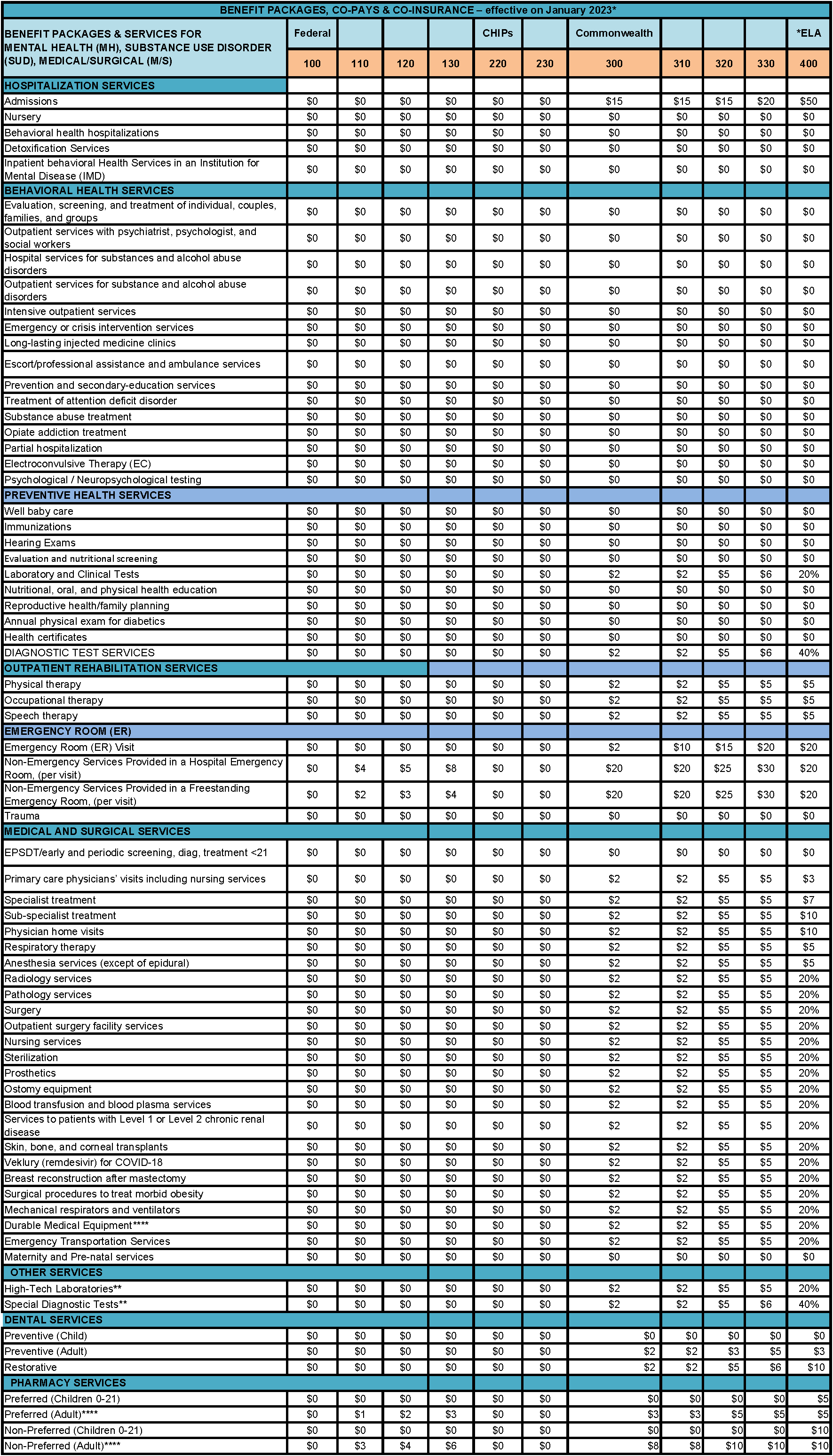
** Copays apply to diagnostic tests only. Copays do not apply to tests required as part of a preventive service.
*** Copays apply to each medicine included in the same prescription pad.

